Category: Cough
-

Breathing Easy: 5 Affordable Ways to Improve Asthma Care in 2024
When it comes to medical treatment, there are often times when technology and research have advanced far beyond what was available decades ago. Asthma treatments are no exception, yet many patients – especially children – continue to be prescribed methods of managing their illness that have been in use for more than 30 years. This…
-

The Hidden Dangers of Ozone: Coping with Ozone Allergies in Summer
Is ozone harmful to your health?
-

How To Avoid Allergies
Suffering from seasonal allergies can be an incredibly unpleasant experience for many people, and the wide range of available treatment options can prove quite daunting. However, there are some steps you can take to help prevent allergen exposure in the first place- ensuring that your environment is free of harmful triggers and forming a routine…
-

How Allergic Sensitization Works–
What Causes Allergies? Are allergies becoming more common? It seems like allergies are increasingly affecting people of all ages. Factors such as climate change, increased exposure to certain allergens, and genetic predisposition could be contributing to this increase in sensitivity. Whether it’s seasonal sneezing or a serious food allergy, understanding the causes of sensitization to…
-

How Snowstorms May Affect Your Asthma
Don’t let cold weather ruin your fun!
-

This Can’t Be Right
So what is going on with persistent allergy symptoms when the pollens are NOT very high? This patient is using the term “allergies” to describe “symptoms” of allergy that may not be IgE-mediated allergy at all. Doesn’t mention skin testing, but this testing can be completely negative in this scenario. How frustrating! In fact, often…
-

Reddit Has It All
Not sure I want to rinse my nose everyday for sinus problems, but here goes. I advise rinsing the nose for chronic sinusitis every day, but patients initially turn their nose up at this suggestion (pun intended). I find myself intrigued at the interest in nasal irrigation, flushing, or whatever else you want to call…
-
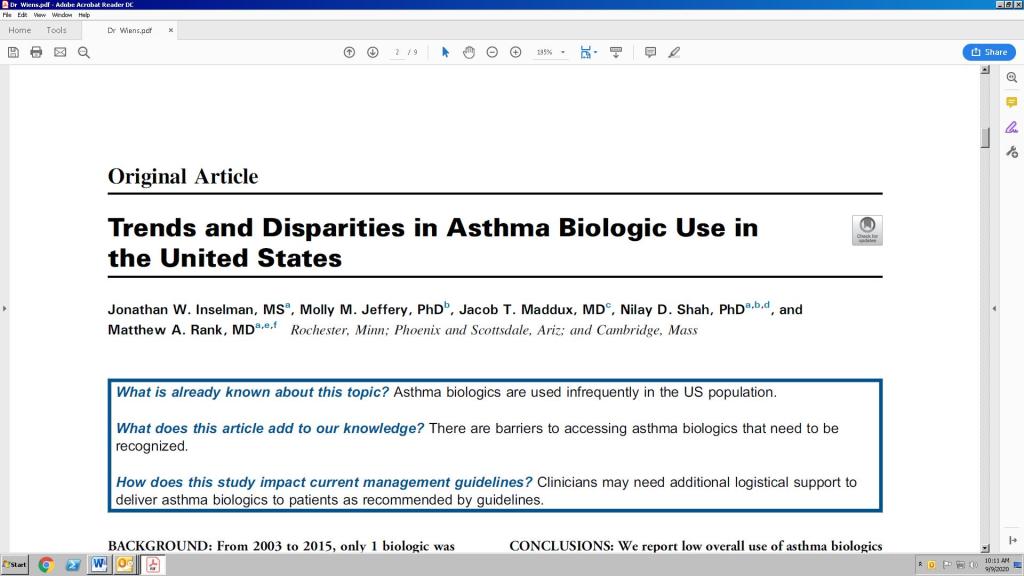
Why Don’t More Patients with Asthma Use Biologicals?
Last month, I shared several videos with you that pertained to treatment of #asthma with biologicals. I hope you listened to the lives of patients just like you who can now “do life” with their family and friends not having to fear the next asthma attack. But it’s not so easy to change our habits…
-

New Biologicals are unknown
What is the magic bullet of medical treatment? How about a biological that treats two or more diseases at one time? Dupilumab (Dupixent) is one such medication and I agree with Dr. Castro’s interpretation of the data on dupilumab–after all, he wrote the study. Here’s what I like about Dupixent: Blocks 2 cytokines, both IL-4…
-
Time for correct use of spacers
Ok..it’s time we learn the “why” of using spacers, because most patients don’t use them on a regular basis. Spacers do several things for your pocketbook and your asthma: This spacer below can be purchased for < $10 on-line at Amazon. That’s almost better than a used toilet roll cardboard! Yes, we used to use…
