Category: Nothing to sneeze at….
-

The Hidden Dangers of Ozone: Coping with Ozone Allergies in Summer
Is ozone harmful to your health?
-

The Need for Speed: How to Get Back to Patients Quickly
So here I am, it’s Monday and Inboxes are full of messages that need replies. We’ve all been there. You visit your doctor’s office for a routine check-up or to address a concerning health issue, only to leave feeling frustrated because you didn’t get the information you needed, or the doctor seemed to be in…
-

Understand the connection between gas stoves and asthma
If you are an asthma or allergy patient, chances are you have been avoiding using a gas stove. After all, reports have suggested that cooking on these stoves could be triggering your allergies and leaving you with uncomfortable—and possibly dangerous—symptoms like coughing, sneezing, or headaches. However, before deciding to avoid using a gas stove altogether,…
-

How To Avoid Allergies
Suffering from seasonal allergies can be an incredibly unpleasant experience for many people, and the wide range of available treatment options can prove quite daunting. However, there are some steps you can take to help prevent allergen exposure in the first place- ensuring that your environment is free of harmful triggers and forming a routine…
-
I Can’t Get My Allergist to Diagnose Allergy!
I’m told I don’t have allergy, but I know that’s not true!
-
What question do patients ask even during their first visit with me?
Making the diagnosis of asthma is tough for both patient and doctor. As an asthma specialist, I can tell you that patients want to know, “doc, when can I stop my medications?” This is often the first question they ask! Ruth Holroyd takes a very candid look at natural treatments for allergic asthma and I…
-
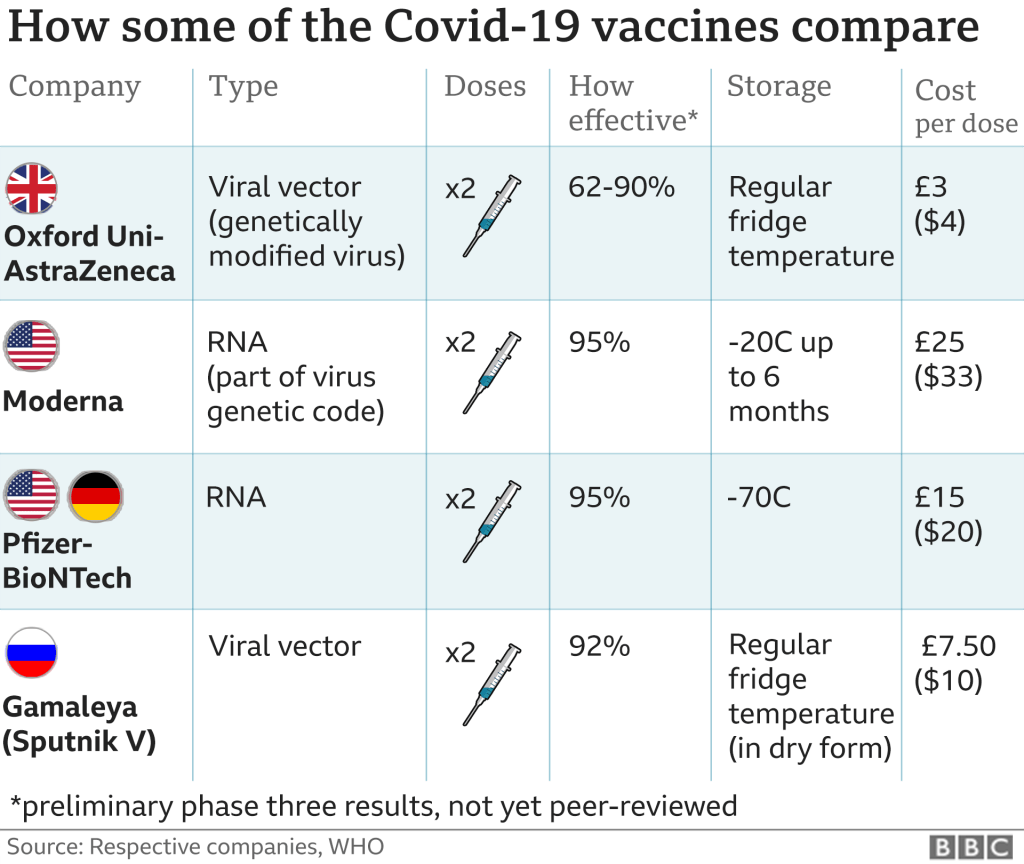
COVID Conundrum
Our hot topics and angry controversies about not only COVID infections but now COVID vaccinations reached the boiling point this past week, resulting in protests over COVID vaccination mandates all over the world. Organized medicine (ie, the AMA) has been accused of covering up the origins of the virus and now the side effects of…
-

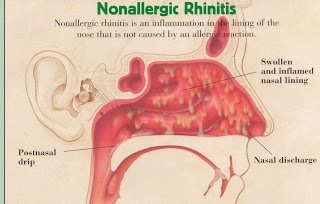
Capsaicin for Nonallergic Rhinitis
February 5, 2021 by Alan Khadavi Here’s the full update and thank-you Alan for sharing Capsaicin nasal spray may be an effective treatment for patients who have nonallergic rhinitis. A significant proportion (25-30%) of patients suffering from rhinitis have nasal symptoms without an infection or allergies, this is referred to nonallergic rhinitis. Up to 50% of these…
-

The Cat’s Out of the Bag!
As the holidays approach, our travel will be limited by #COVID-19, but we still may visit relatives with #cats, and you’re allergic! Researchers from Nestle Purina Research in St Louis MO may have part of the answer. As cats groom (which they do all the time), Fel d 1 is distributed within the hair coat…
-

It’s a scam to our patients
Much of my medical office day is explaining to patients what they DON’T have rather than treating #allergy. Allergy has become the explanation for all medical disease. For instance, it’s rare for allergy to cause lack of attention, abdominal cramping (because of food allergy), or even constipation, but patients want allergy testing nonetheless. What are…
