Much of my medical office day is explaining to patients what they DON’T have rather than treating #allergy. Allergy has become the explanation for all medical disease. For instance, it’s rare for allergy to cause lack of attention, abdominal cramping (because of food allergy), or even constipation, but patients want allergy testing nonetheless. What are some “non-allergy” conditions that you’re likely to spend money you don’t need because of excessive testing?
This writing, however, isn’t about COVID-19 (that’s in a previous blog). Granted, all you see on social media and mainstream media today is COVID, COVID, COVID. We should take COVID-19 very seriously-our COVID numbers aren’t looking good (many days in Oklahoma > 1,000), but other diseases cause coughing and wheezing especially during the winter that aren’t “the virus”. In fact, if you have a “cold” that lasts longer than one week, you may be experiencing a sinus infection rather than a virus anyway. Treatment for sinus infections often require antibiotics and steroids (in the form of prednisone) for 4-6 weeks to completely resolve your infection. But if you’re concerned about COVID, testing to exclude COVID-19 is readily available, and I’ve mentioned previously how to distinguish allergy from COVID. Now there’s a test to check yourself from a home sample. It doesn’t get any easier than that! Home COVID testing

Food allergy is another one of those “allergy issues” that gets a lot of attention, but many times isn’t correct. Patients are desperate for food to contribute to their symptoms. The diagnosis of anaphylactic food reactions rose 377 percent from 2007 to 2016, according to an analysis that FARE commissioned from FAIR Health, a national, independent, nonprofit organization that collects and analyzes data on healthcare costs, including food testing. If only my investments did this well! Specifically in Oklahoma, the top 5 foods causing anaphylactic reactions were eggs, peanuts, and tree nuts/seeds. Unfortunately, most of the foods in all 51 states that caused anaphylaxis were unidentified or classified as “other”. One of the major problems with food allergy is many times we really have no idea which foods are really causing the problem. But does this keep people from looking for the next best food testing? Noooo– Look no further than Google.
- Searches for food allergy testing came in at 155 million
- Asthma which has a much higher economic impact on school attendance, work performance was much less of a desirable search destination coming in at 105 million
- Allergic rhinitis or “hayfever” didn’t seem very exciting with only 12.3 million searches on Google
Although interest in #food allergy testing has skyrocketed, the diagnosis of food allergy remains the same: food ingestion history and elimination/challenge testing. What I mean by this is simple, but not easy. If you (or your child) can tolerate eggs without any hives, or difficulty breathing, you probably don’t have a food allergy. If testing is positive, that means you have SENSITIVITY but not necessarily food allergy. You’ve ingested the food before, and testing will tell you that but don’t read too much into the results. Try not to pay for expensive testing, when all you need is a good food history. Elimination/challenge testing is quite similar–take out the food in question from your diet (let’s say milk) and if you’re symptoms of allergy don’t get better, you can probably continue consuming milk without difficulty. Add the milk back in and if your allergies don’t worsen, you prove to yourself and your doctor, that milk is not one of your allergies. It’s interesting to note that food allergies are not “hidden” triggers and the reactions are generally not delayed for more than 1-2 hours. In other words, food you consumed last night won’t cause your headache in the morning.
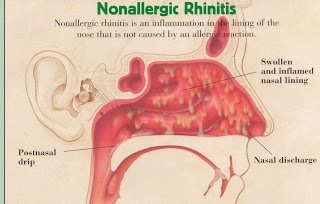
Non-allergic rhinitis. What do you say when someone has no allergy and testing is all negative? I can sum up why you don’t have allergy in one word: IgE. Patients with allergy have lots of #IgE floating around and can join to pollens in order to create the reaction of sneezing, runny nose, and congestion that you’re all familiar with. Beware, not everyone has allergy, and testing for allergies is the only time when patients are disappointed with a negative test. Imagine if you’re disappointed when your cardiac catheterization comes back clean–darn, I don’t have heart disease. Can you feel the sarcasm? Granted, you don’t improve with allergy shots unless you have positive testing to begin with, but there are many effective medications to stop that runny nose even if you don’t have allergies. It’s been requested by readers to include more information about Atrovent or ipratropium and I’ll plan on that in the near future. But for now, that’s another day.
What a lead into the next topic of potential deception–chronic sinusitis. Now is the sinus season during the holidays and most patients are completely unaware that the “cause” of runny nose and congestion is no longer allergy, but has switched to sinus infection. Using allergy medications like Zyrtec, Claritin, or Allegra will not improve a #sinus infection if there are no allergies in the air. Just look at pollen counts during November, December, and January–only moderate molds and nothing else. You may experience “allergies” but without pollen in the air, you’ve likely been fooled by the sinus bug. Sometimes, a CT scan of the sinuses will uncover the problem; many times it takes one month of antibiotics & corticosteroids to resolve the infection. Remember, colds last ~ 1 week and anything longer may be your sinuses. In any event, I’ve exceeded my word limit for this entry; please don’t ruin your holidays with undiagnosed sinus infection. Get to the root of your allergy problem fast, and enjoy Turkey Day and Christmas. Until next time,



