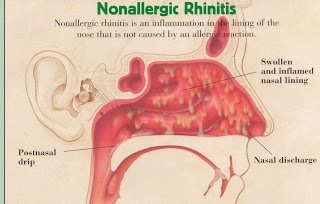
Category: Vasomotor (Non-allergic) Rhinitis
-

Understanding Skin Testing Methods for Allergies
Which one (skin testing or blood testing) should I do?
-
I Can’t Get My Allergist to Diagnose Allergy!
I’m told I don’t have allergy, but I know that’s not true!
-

It’s a scam to our patients
Much of my medical office day is explaining to patients what they DON’T have rather than treating #allergy. Allergy has become the explanation for all medical disease. For instance, it’s rare for allergy to cause lack of attention, abdominal cramping (because of food allergy), or even constipation, but patients want allergy testing nonetheless. What are…
-
Myth-busters in Medicine
As an allergist in Tulsa, the myths that surround asthma, food allergy, hives, hay fever abound and patients often come in to the office telling ME what they are allergic to or how to fix the problem. Let me give you some examples:
-
Where Do You Get Your Medical Information?
I recently found an article on the accuracy of #medical information on #Facebook–it was 85% (wrong that is). With this much misinformation at our fingertips, no wonder medical advances seem to be muted…obesity, cost of medical care, gun violence, heart disease. If you’re relying on the internet for your medical information, perhaps this link on…
-
Dear Doctor…..
Dear Doctor, Thanks for all your help with my #allergies, but I have a bone to pick with you. A few minutes into my visit and you’re talking about “rhinitis” and “IgE” and “desensitization”. By the time my brain catches up with you, our visit is over and I don’t feel like I really…
-
Tulsa is the Allergy Capital of the Nation
Tulsa is the #allergy capital of the nation. You wouldn’t believe how many times in a day I hear that! and it makes sense…countless numbers of patients return to Tulsa and find their #allergies are now out of control. But is this really true? Does anyone even keep track of which city in America has the…
-
Put This Myth to Rest-(Dirt Jet Pro/SCRUBS hand sanitizer wipes)
Everyday I teach patients the difference between “allergy” and “irritant” reaction. TV ads are overloaded with allergy advertisements in an attempt to sell antihistamines, so why wouldn’t you think that everyone has allergy of some kind. The link below is a question about allergy (anaphylaxis in this case) to chemicals. Consider the following: Adverse reactions…
-
Air fresheners–Go Organic…Not!
Tomorrow starts the American Academy of Allergy, Asthma, & Immunology national meeting in Orlando. Great fun and food, but more importantly, great new information about allergy. If you watch the news at all, you’re bound to hear about natural products for your health. Organic anyone? Read this blog about a patient who only THOUGHT she had allergy;…
-
Now Here’s a New Medication I haven’t seen in a while
I have trouble getting patients to use ONE much less TWO nasal sprays for nasal allergy & congestion. Now I may have a solution this year. The buzz on the street is Meda pharmacueticals will be introducing a nasal spray product with two ingredients for patients suffering from congestion, runny nose and sneezing. Yes, for what…
