Tag: Asthma
-
Could We “Turn Off” Allergies With Gene Editing? Here’s What CRISPR Actually Makes Possible
A baby with a fatal metabolic disorder was successfully treated with CRISPR gene editing, raising hopes for managing allergies. However, allergies involve complex genetic and environmental factors, making CRISPR a challenging solution. The future may include targeted treatments for immune disorders, but widespread applicability for allergies remains uncertain and ethically debated.
-

Spring Sneezes Are Starting Earlier Every Year. Here’s What That Means for You:
Spring allergy symptoms are starting earlier each year, with increased pollen counts leading to severe discomfort. To prepare, begin using nasal steroid sprays early, track local pollen levels, and maintain a clean indoor environment. Allergy shots can help reduce long-term sensitivity. Effective preparation can significantly improve the spring experience.
-

How Weight-Loss Drugs and AI Are Reshaping Allergy Medicine
In 2026, GLP-1 drugs and AI are transforming allergy care. While GLP-1 medications alter appetite signaling and aid weight loss, the potential for allergic reactions complicates patient experiences. AI enhances diagnostics by streamlining processes and improving accuracy, ultimately leading to better outcomes and fewer misdiagnoses in allergy treatments.
-

Women, Hormones, and Allergies: Why Your Symptoms Change and What to Do About It
Allergies exhibit different patterns in women and men, largely influenced by hormones. After puberty, estrogen increases allergy risk, causing symptoms tied to menstrual cycles and pregnancy. Understanding hormonal patterns can help women manage these flares with proactive treatment strategies, rather than reactive responses, improving overall quality of life through various life stages.
-
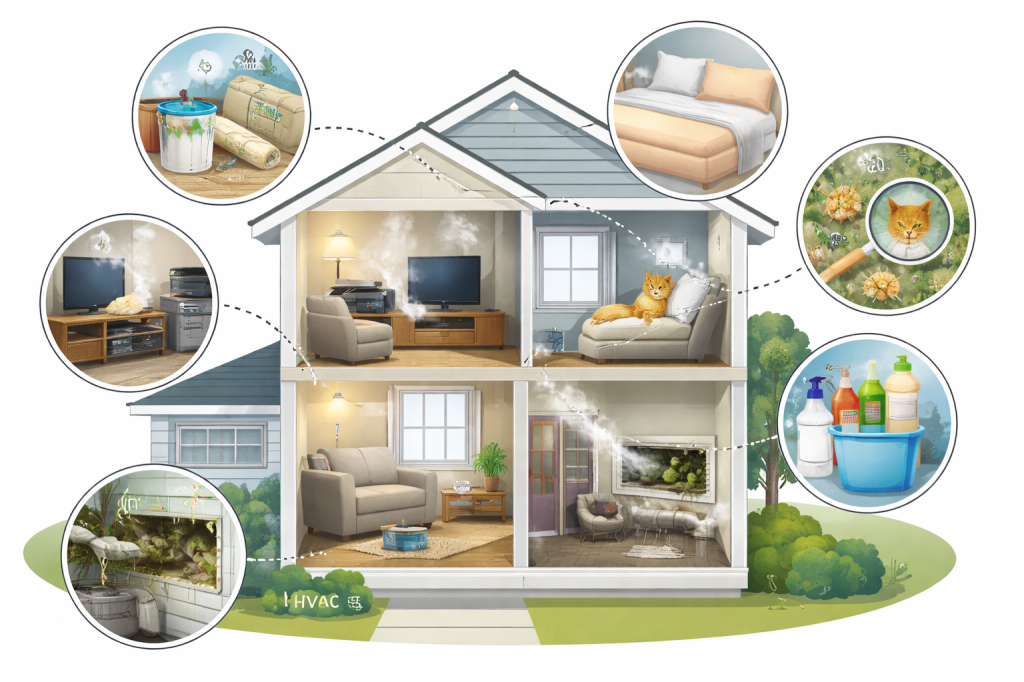
Hidden Allergens in the Home: What’s Really Irritating Your Body
Allergies are often underestimated as indoor problems, with volatile organic compounds (VOCs) and mold being significant irritants. VOCs are released from everyday items like carpets and electronics, while mold proliferates in HVAC systems. Both contribute to chronic respiratory issues, prompting the need for effective measures to improve indoor air quality and humidity management.
-

The Seed Oil–Allergy Link No One’s Explaining Correctly
Seed oils face criticism as a potential cause of health issues like inflammation and allergies. However, not all seed oils are harmful; those high in omega-6 fats can increase allergic sensitivity, while omega-3-rich oils can help reduce it. Making informed choices can significantly impact health and allergy symptoms over time.
-
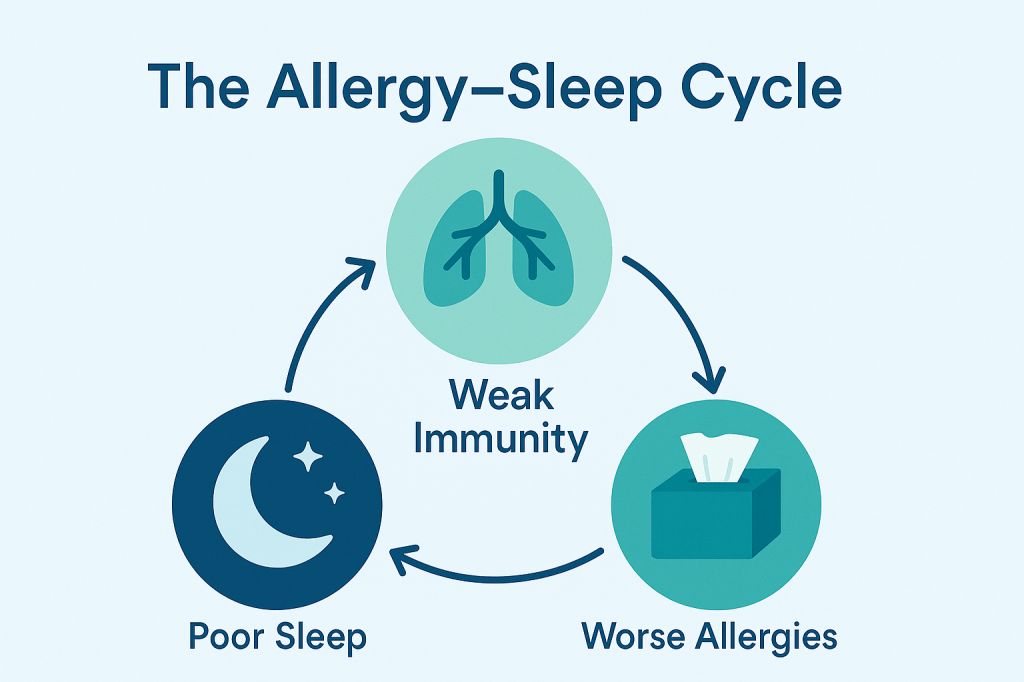
The Overlooked Connection Between Sleep and Allergies
Many overlook the link between sleep and allergies, but poor sleep can worsen allergic symptoms and overall immune function. Poor sleep leads to increased inflammation and allergic reactions. Improving sleep hygiene can alleviate allergy symptoms significantly, emphasizing the importance of prioritizing restful sleep as a key component of allergy management.
-

Hidden Allergens in Popular Diets: What You’re Overlooking (and How to Fix It)
The shift toward diets like keto, vegan, and paleo introduces hidden allergens that can pose serious risks. Reformulations in packaged foods, cross-contact during food preparation, and mismanagement of allergies complicate safety. It’s essential to be vigilant about ingredient changes and maintain a food diary to distinguish between true reactions and dietary adjustments.
-

The Overlooked Link Between Obesity and Allergies
When people talk about obesity, the conversation almost always stops at diet and exercise. Calories in, calories out. Move more, eat less. But here’s what almost no one mentions: obesity throws your immune system into overdrive. Every 5-point increase in BMI raises asthma risk by about 30%, and obese patients report worse control, more flare-ups,…
-

The Allergy Crisis No One in Public Health Wants to Talk About
Allergy rates have risen dramatically in the past 30 years, largely due to the hygiene hypothesis, which limits immune system exposure to microbes. Climate change also worsens allergies, while socioeconomic factors complicate the issue. Public health efforts prioritizing education, local pollen counts, and preventive measures could significantly reduce allergy-related healthcare costs and improve outcomes.
