Tag: Asthma
-

The 7 Mistakes I Made Early in My Allergy Practice—And What I Do Differently Now
I’ll be honest: I built my allergy practice by stumbling first. I overpaid hospitals, underpriced visits, and clung to old protocols long after the data moved on. Here is the short version so you can skip the bruises—what I did wrong, what I do now, and the simple steps to copy this week. 1. I…
-

The Biggest Breakthroughs in Allergy Research This Year
Most allergy treatments still play defense. You react, you medicate, and then you wait for it to come back. But this year? We’re finally playing offense. From food allergies to eczema to asthma, the latest breakthroughs are revolutionizing the entire field. Here’s what’s new and what you can do about it right now. 1. Biologics…
-
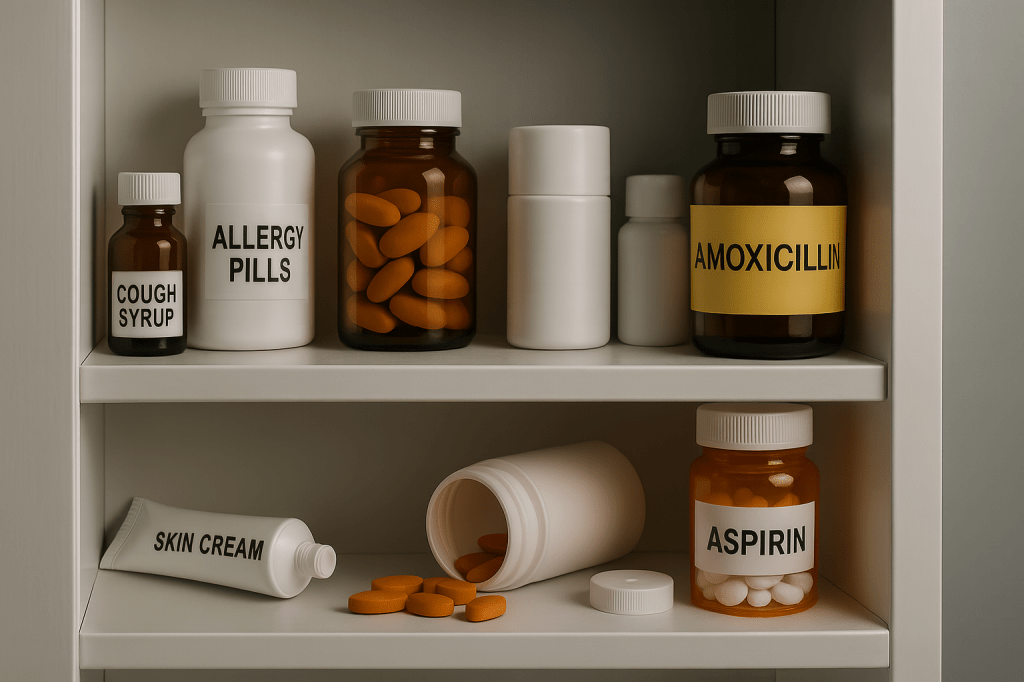
The Top Allergy Triggers Lurking in Your Medicine Cabinet
Your medicine cabinet may contain allergy triggers, including leftover antibiotics, over-the-counter pain relievers like ibuprofen, topical creams, and inactive ingredients. Reactions can be immediate or delayed. Always use familiar medications, avoid sharing, and consult an allergist if you experience symptoms. Regularly clean and organize your cabinet for safety.
-

When Allergies and Eczema Collide: Understanding the Atopic March
The atopic march refers to the progression of allergic conditions in children, typically beginning with eczema or food allergies and potentially leading to asthma. Early detection and intervention, including testing IgE levels, tracking triggers, and consulting an allergist, are crucial to managing these conditions and preventing further complications.
-

OpenEvidence AI in Allergy Care: The Best Assistant I Didn’t Know I Needed
Allergy care is complex, but OpenEvidence AI simplifies the documentation and research process for doctors. It enables rapid access to evidence-based answers, reduces errors, saves time, and enhances patient trust through transparency. This AI tool is transforming practices, decreasing burnout, and paving the way for a future where AI integrates seamlessly into medical care.
-

The Future of Asthma Biologics: What Every Patient (and Parent) Needs to Know
Biologics are transforming asthma treatment by targeting specific inflammatory molecules instead of broadly suppressing the immune system, leading to fewer medications and reduced emergency visits. While expensive, insurance can often cover them with proper navigation. Their benefits include improved lung function and less reliance on daily medications, making asthma management more manageable.
-

10 Tips for Parents of Kids With Asthma (From a Doctor Who’s Seen It All)
Approximately 4.9 million American children have asthma. Effective management involves ongoing treatment, understanding triggers, preparing for school, and creating an action plan. Proactive measures help ensure kids lead active, healthy lives despite their condition.
-

Top 10 Asthma Myths You Need to Know
Asthma still kills. Roughly 3,500 people die from asthma in the U.S. each year. This is not because it’s untreatable, but because it’s misunderstood. Bad information leads to bad decisions, which can cost you your life. Here’s what every asthma patient needs to know: 1. Asthma is just a childhood disease Not even close to…
-

Why Food Allergy Rates Are Rising—and What It Means for Public Health
Food allergies are skyrocketing. Since 1997, peanut allergies in children have tripled, and food allergies overall have increased by 50%. It’s not just an individual health issue; it’s a $25 billion-a-year problem when you factor in rising emergency room visits, increased medications, lost productivity, and special dietary needs. While advancements in emergency treatment have helped…
-

Breathing Easy: 5 Affordable Ways to Improve Asthma Care in 2024
When it comes to medical treatment, there are often times when technology and research have advanced far beyond what was available decades ago. Asthma treatments are no exception, yet many patients – especially children – continue to be prescribed methods of managing their illness that have been in use for more than 30 years. This…
